

3. April 2026
physiotherapy for sciatica: a complete guide to treatment, exercises & recovery
Physiotherapy is the recommended first-line treatment for sciatica, with around 60% of patients recovering within six weeks through structured exercise, manual therapy, and nerve mobilisation techniques. At CK Physio in West London, our Chartered Physiotherapists use personalised, evidence-based programmes to reduce sciatic pain, restore mobility, and help you return to normal activity — whether at our Hanwell clinic or through home visits across Ealing and the surrounding area.
What Is Sciatica and What Causes It?
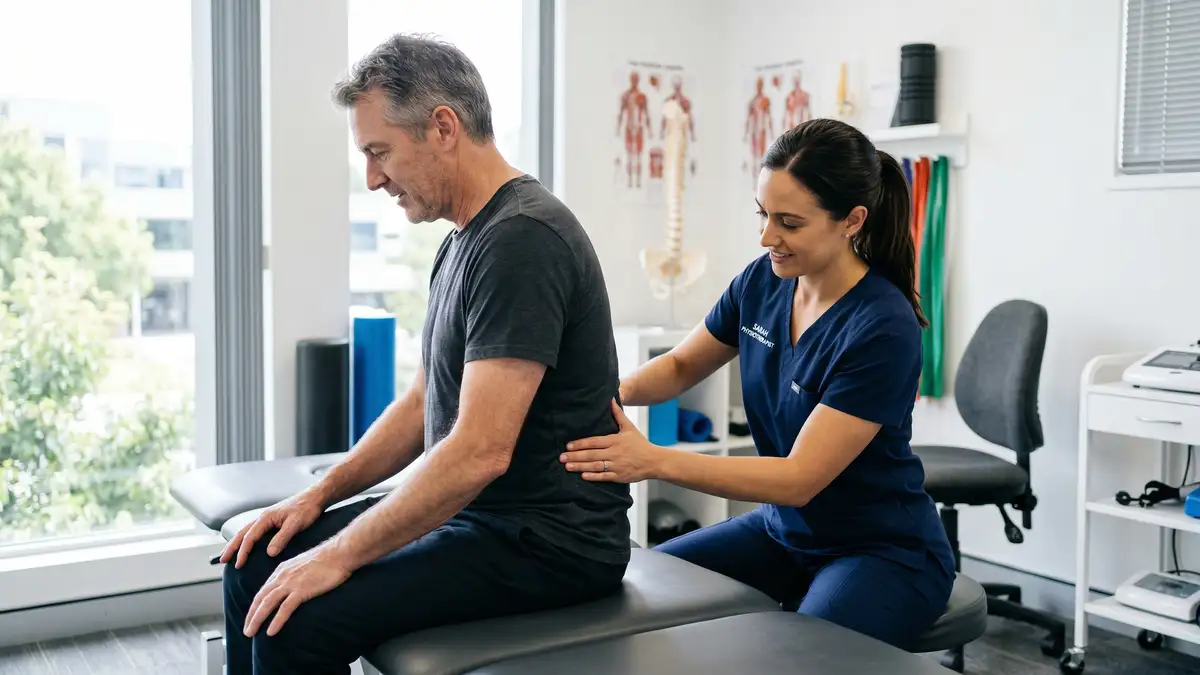
Sciatica describes radiating pain that travels from the lower back or buttock down the leg, caused by compression or irritation of the sciatic nerve — the largest nerve in the body, formed from nerve roots L4 through S3. The pain is often described as a sharp, shooting, or electric shock sensation that can extend all the way to the foot or toes.
The most common cause of sciatica is a lumbar disc herniation, where the soft inner material of a spinal disc presses on a nearby nerve root. Around 40% of people with radiating leg pain have disc herniation as the underlying cause. Other common causes include spinal stenosis (narrowing of the spinal canal, particularly in adults over 50), degenerative disc disease, spondylolisthesis, and piriformis syndrome — where the piriformis muscle in the buttock compresses the sciatic nerve.
Risk factors for developing sciatica include prolonged sitting (which increases pressure on lumbar discs by up to 40% compared to standing), obesity, age-related spinal changes, diabetes, and certain occupational factors such as heavy lifting or driving for extended periods. In the UK, sciatica affects approximately 2.2% of the population annually, with lifetime prevalence estimated between 13% and 40%.
2.2%
UK Annual Prevalence
Proportion of UK adults affected by sciatica each year
£12.4bn
Annual UK Cost
Total healthcare and productivity costs of sciatica
60%
Recovery in 6 Weeks
Patients recovering with conservative physiotherapy care
13–40%
Lifetime Prevalence
Proportion of people who will experience sciatica
Sources: Ridsdale et al. 2025 (PMC), British Medical Journal cited evidence
| Cause | What Happens | Who It Affects | Physiotherapy Approach |
|---|---|---|---|
| Disc Herniation | Soft disc material presses on a nerve root — the most common cause (approx. 40% of cases) | Adults 20–50, often after lifting or twisting | McKenzie extension exercises, nerve mobilisation, core stabilisation |
| Spinal Stenosis | Narrowing of the spinal canal compresses nerve roots, often gradually | Adults over 50, age-related degeneration | Flexion-based exercises, mobility work, manual therapy |
| Piriformis Syndrome | Piriformis muscle in the buttock compresses the sciatic nerve (5–8% of back pain cases) | Runners, desk workers, those with hip tightness | Piriformis stretching, soft tissue release, shockwave therapy |
| Spondylolisthesis | One vertebra slips forward over another, narrowing the nerve exit space | Athletes, older adults with degenerative changes | Core stabilisation, posture correction, activity modification |
| Degenerative Disc Disease | Age-related disc wear reduces disc height and may irritate nearby nerves | Adults 40+, gradual onset | Strengthening exercises, manual therapy, ergonomic advice |
Sources: NICE NG59, NHS Sciatica Overview
How Do You Know If You Have Sciatica?
Sciatica typically presents as pain radiating from the lower back or buttock down the back or side of one leg, potentially reaching the foot. Unlike simple lower back pain, sciatica follows the path of the sciatic nerve and often produces additional neurological symptoms including numbness, tingling, or a "pins and needles" sensation along the affected leg.
The character of sciatic pain varies between individuals — it may feel like a sharp, burning, or shooting sensation that worsens with coughing, sneezing, or prolonged sitting. In more severe cases, muscle weakness may develop in the affected leg or foot. Foot drop (difficulty lifting the front part of the foot) can occur when the L5 nerve root is involved, while S1 nerve root compression may cause weakness in pushing off during walking.
When to Seek Urgent Medical Attention
Cauda equina syndrome is a rare but serious condition requiring emergency care. Seek immediate medical help if you experience: sudden loss of bladder or bowel control, numbness in the saddle area (inner thighs, backs of legs, around the buttocks), sudden severe weakness in both legs, or rapidly worsening neurological symptoms.
These symptoms may indicate compression of the nerves at the base of the spinal cord and require urgent assessment — typically within hours, not days.
Physiotherapists use several clinical tests to assess sciatica during an initial consultation. The straight leg raise test (Lasègue's test) involves slowly lifting the extended leg while you lie on your back — reproduction of your familiar leg pain between 30 and 70 degrees suggests sciatic nerve involvement. The slump test combines spinal flexion with leg movements to assess the sciatic nerve under more functional conditions. A full neurological examination including strength testing, sensation assessment, and reflex checks helps identify which nerve root is affected and guides treatment planning.
Imaging such as MRI is not routinely needed for sciatica. The NICE guideline NG59 recommends considering imaging only when symptoms persist beyond six weeks despite appropriate treatment, when there are progressive neurological deficits, or when red flag conditions are suspected. Importantly, many people without any back or leg pain show disc bulges or herniations on MRI scans, so imaging findings must always be interpreted alongside clinical symptoms.
Key Takeaway
Sciatica is diagnosed primarily through clinical assessment, not imaging. A skilled physiotherapist can identify the likely cause and affected nerve root through physical examination, enabling treatment to begin promptly — often within days rather than the weeks or months required for NHS MRI referrals.
How Does Physiotherapy Treat Sciatica?
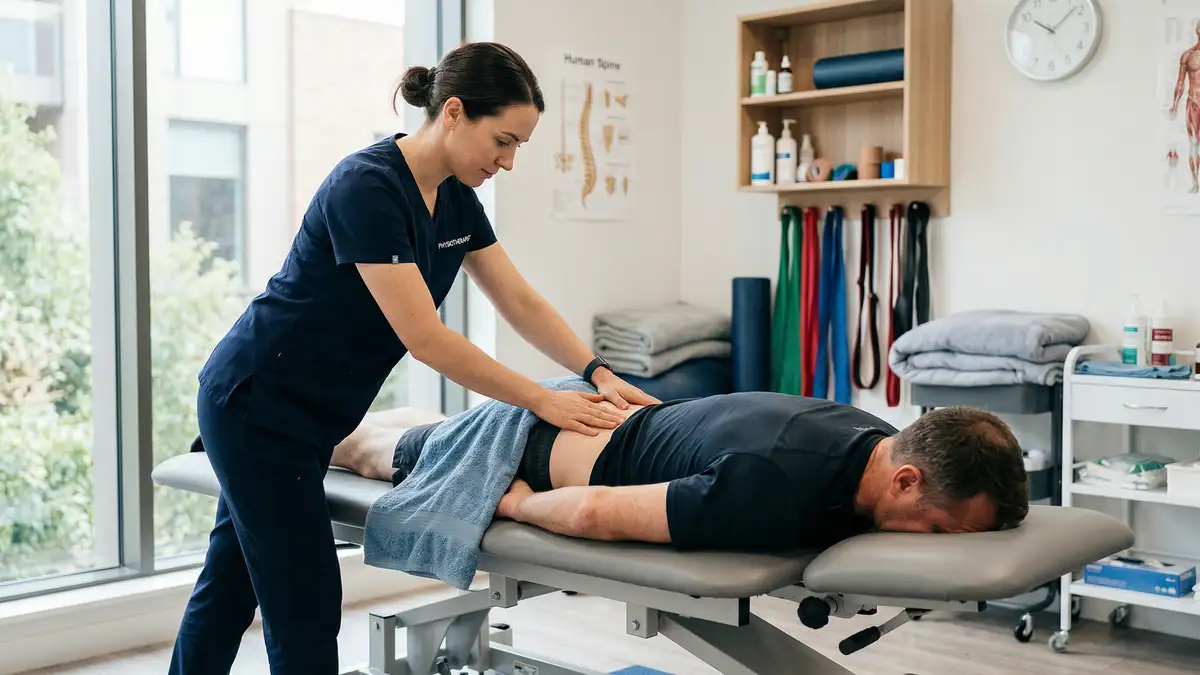
Physiotherapy for sciatica combines several evidence-based approaches tailored to the underlying cause, severity, and stage of your condition. The NICE guideline NG59 recommends physiotherapy and exercise as first-line treatment for sciatica, with research demonstrating that early access to structured physiotherapy produces better outcomes than delayed intervention or usual care alone.
Manual Therapy and Spinal Mobilisation
Manual therapy techniques used by CK Physio's Chartered Physiotherapists include soft tissue massage to reduce muscle tension around the affected area, spinal joint mobilisation to improve movement in stiff spinal segments, and specific techniques to address joint restrictions contributing to nerve compression. These hands-on approaches help reduce pain, improve spinal mobility, and create better conditions for nerve recovery.
The McKenzie Method (Mechanical Diagnosis and Therapy)
The McKenzie method is a structured assessment and treatment approach widely used for spinal conditions including sciatica. It focuses on identifying your "directional preference" — the specific movement direction that reduces or centralises your symptoms. Research shows that 58% to 91% of people with lower back pain experience centralisation of symptoms through McKenzie-based exercises, with the majority responding to extension-based movements. Studies demonstrate low-to-moderate certainty evidence that the McKenzie method reduces pain for up to six months and disability for up to 12 months in patients who show a directional preference.
Nerve Mobilisation and Gliding Techniques
Neural mobilisation (sometimes called nerve gliding or nerve flossing) involves gentle, controlled movements designed to improve the sciatic nerve's ability to slide within its surrounding tissues. A randomised controlled study found that neurodynamic sciatic nerve sliding techniques improved hamstring flexibility significantly — with straight leg raise increasing from 79° to nearly 92° after treatment — alongside improvements in balance. At CK Physio, nerve mobilisation techniques form a key part of sciatica rehabilitation once acute compression has been addressed, helping restore normal nerve movement and reduce sensitivity.
Core Stabilisation and Therapeutic Exercise
Exercise therapy is a cornerstone of sciatica physiotherapy. A comprehensive meta-analysis found that core stability exercises produced large pain reduction effects (standardised mean difference of −0.90) compared to moderate effects from general spinal stability exercises. Programme duration matters significantly — six-week programmes show moderate effects, while eight-to-twelve-week programmes produce large effect sizes supported by high-quality evidence.
The specific exercises prescribed depend on the underlying cause of your sciatica. For disc-related sciatica, extension-based exercises (such as the prone press-up) help centralise symptoms. For stenosis-related sciatica, flexion-based exercises (like knee-to-chest stretches) may provide greater relief by opening the spaces through which nerve roots exit the spine. CK Physio's physiotherapists design individualised exercise programmes matched to your specific diagnosis, ensuring you perform the right movements for your condition.
| Treatment Approach | Evidence Summary | Best For |
|---|---|---|
| McKenzie Method | Reduces pain up to 6 months, disability up to 12 months in patients with directional preference | Disc-related sciatica with centralisation response |
| Core Stabilisation | Large pain reduction effect (SMD = −0.90); 8–12 week programmes most effective | All sciatica causes; essential for long-term prevention |
| Nerve Mobilisation | Improves nerve flexibility and postural balance; SLR improved from 79° to 92° | Post-acute sciatica once compression is managed |
| Manual Therapy | Reduces pain and improves mobility; most effective combined with exercise | Stiff spinal segments, muscle tension contributing to nerve irritation |
| Electrotherapy (TENS/IFT) | Provides temporary pain relief; deeper penetration with interferential therapy | Adjunctive pain management alongside active rehabilitation |
| Acupuncture | Promising for pain reduction (RR = 1.23); further high-quality research needed | Complementary approach for chronic or persistent sciatica |
Sources: Dimitrijević et al. 2025, Mann et al. 2023 (StatPearls), Park et al. 2014
Does Physiotherapy Work Better Than Surgery for Sciatica?

This is one of the most common questions patients ask, and the evidence provides a clear answer: physiotherapy and surgery produce comparable long-term outcomes for most sciatica cases. A 2025 meta-analysis examining randomised controlled trials found that surgery provided faster pain relief in the short term (first two to six months), but by 12 to 24 months, outcomes between surgical and conservatively managed patients converged to similar levels.
The specific disability improvements from surgery were modest at six months — with mean differences of approximately 3 points on the Roland Morris Disability Questionnaire and 5 points on the Oswestry Disability Index — and these differences were neither statistically nor clinically significant at longer follow-up periods. This evidence strongly supports a physiotherapy-first approach, with surgery reserved for patients who do not respond adequately to four to six months of structured conservative care.
Surgery becomes the appropriate option when there are progressive neurological deficits (worsening weakness or loss of function), symptoms of cauda equina syndrome, or when six months of well-managed physiotherapy has not produced sufficient improvement. Importantly, research shows that patients who do eventually require surgery achieve better outcomes when the operation is performed within six months of symptom onset, which underscores the importance of early physiotherapy assessment and monitoring — not watchful waiting.
The Bottom Line
Physiotherapy produces outcomes comparable to surgery at one to two years — without the risks of anaesthesia, infection, or extended post-operative recovery. At CK Physio, we monitor your progress closely and can advise on the right time to consider specialist referral if conservative treatment is not achieving the results we expect.
Struggling with sciatica? Our Chartered Physiotherapists can assess your condition and create a personalised treatment plan — at our clinic or in your own home.
Book Your AssessmentHow Long Does Sciatica Take to Recover?
Recovery timelines for sciatica vary depending on the underlying cause, severity of nerve compression, and how quickly treatment begins. Understanding these stages helps set realistic expectations and ensures you stay on track with your rehabilitation programme.
Acute Phase (0–4 Weeks)
Significant inflammation around the compressed nerve. Many acute cases begin improving within days to weeks with appropriate physiotherapy. Focus is on pain management, gentle movement, and avoiding aggravating activities. Around 60% of patients with acute sciatica recover within six weeks using conservative care.
Subacute Phase (4–12 Weeks)
Ongoing nerve irritation with gradually reducing symptoms. Treatment progresses to more active rehabilitation — core stabilisation exercises, nerve mobilisation, and functional movement training. Most patients see substantial improvement during this phase with consistent physiotherapy.
Chronic Phase (12+ Weeks)
Symptoms persisting beyond three months may indicate unresolved structural issues. This is a critical decision point — early, appropriate physiotherapy intervention within the first three to six months helps prevent the transition to chronic sciatica. If improvement has plateaued, your physiotherapist may recommend specialist review or imaging.
Return to Full Activity
Most patients return to normal activities within three to six months. Up to two-thirds of herniated discs naturally shrink as the body reabsorbs the disc material. Your physiotherapist will guide graduated return to sport, exercise, and demanding physical activities using evidence-based progression criteria.
What Can You Do at Home to Relieve Sciatica?
Self-management plays an essential role in sciatica recovery. The exercises and strategies your physiotherapist prescribes for home use are just as important as your clinic sessions — research suggests that high-frequency home exercise (potentially up to 10 repetitions of prescribed movements daily) produces better outcomes than relying solely on supervised sessions.
Movement and Activity
Current evidence strongly supports gentle, early movement over bed rest for sciatica. Even short walks of five to ten minutes promote blood flow, reduce inflammation, and prevent the muscle stiffness and deconditioning that prolonged rest can cause. After the first 24 to 48 hours of strategic rest during an acute flare-up, gradual movement resumption accelerates recovery. Swimming and water-based exercise can be particularly helpful as the water's buoyancy supports the body while allowing full-range movement.
Heat, Cold, and Sleep Position
During the first 72 hours after a sciatica flare-up, ice applied to the lower back (not the leg) for 10 to 20 minutes several times daily helps reduce acute inflammation. After this initial period, heat therapy for 15 to 30 minutes promotes blood flow and reduces muscle tightness. Many people find alternating between ice and heat particularly effective. For sleep, lying on your side with a pillow between the knees maintains spinal alignment, while sleeping on your back with a pillow or wedge under the knees reduces pressure on the lumbar spine. Stomach sleeping should be avoided as it strains the back and can worsen symptoms.
Ergonomic Changes for Desk Workers
If you work at a desk, prolonged sitting is one of the biggest aggravating factors for sciatica. Take movement breaks every 20 to 30 minutes — stand, stretch, or take a brief walk. Ensure your chair provides proper lumbar support and position your monitor at eye level. Standing desk options can help reduce continuous spinal loading. CK Physio offers ergonomic assessments as part of our treatment approach, particularly during home visits where we can evaluate your actual working environment and recommend specific adjustments.

Why Choose Home Visit Physiotherapy for Sciatica?
Acute sciatica can make even short car journeys extremely painful. Sitting in a car increases pressure on the lumbar spine and compressed nerve, often making travel to a clinic impractical during the most acute phase — precisely when early physiotherapy intervention matters most.
CK Physio's home visit physiotherapy service across Hanwell, Ealing, and West London removes this barrier entirely. Our Chartered Physiotherapists bring full assessment and treatment capabilities to your home, meaning you can begin structured rehabilitation without the pain and difficulty of travelling. Home visits also offer a unique advantage: your physiotherapist can assess your actual sleeping position, work setup, and daily movement patterns in context, providing practical ergonomic advice tailored to your specific environment.
With 85% of West London physiotherapy clinics not offering specialist home visit services, CK Physio's home-based sciatica treatment fills a significant gap — particularly for patients who are bed-bound or severely limited in the acute phase, elderly patients for whom travel is difficult, and anyone whose sciatica prevents comfortable driving or use of public transport.
How Does Sciatica Treatment Fit Within the NHS Pathway?
The typical NHS pathway for sciatica begins with your GP, who will assess your symptoms, exclude any red flag conditions, and provide initial advice on pain management and self-care. If symptoms persist, your GP can refer you to NHS community physiotherapy or musculoskeletal services.
The challenge lies in timing. Median NHS waiting times for routine orthopaedic services now exceed 46 weeks, and even physiotherapy referrals can involve waits of several weeks to months depending on your area. Research consistently shows that early physiotherapy access produces superior outcomes — yet the NHS pathway often means treatment begins well after the optimal early intervention window has passed.
Private physiotherapy through CK Physio offers rapid access — typically within days rather than weeks. This means assessment, diagnosis, and treatment can begin during the acute phase when intervention is most effective at preventing chronic sciatica. CK Physio is registered with BUPA and AXA PPP, and our physiotherapists are HCPC-registered and members of the Chartered Society of Physiotherapy, ensuring the same professional standards as NHS services with significantly faster access.
Key Takeaway
Early physiotherapy access is one of the strongest predictors of good sciatica outcomes. Delayed treatment within the NHS pathway increases the risk of chronic pain development. Private physiotherapy through CK Physio provides rapid assessment and treatment — often within days — helping prevent the transition from acute to chronic sciatica.
Can Electrotherapy and Shockwave Therapy Help with Sciatica?
CK Physio offers several complementary treatment modalities that can support your sciatica recovery alongside manual therapy and exercise. Electrotherapy, including TENS (transcutaneous electrical nerve stimulation) and interferential therapy, provides pain relief through electrical stimulation of sensory nerve fibres. Interferential therapy penetrates deeper than standard TENS, targeting the deeper muscle and nerve tissues involved in sciatica. While electrotherapy is best used as an adjunct to active rehabilitation rather than a standalone treatment, it can help manage pain levels sufficiently to enable you to engage more fully in your exercise programme.
Shockwave therapy may be beneficial for sciatica caused by piriformis syndrome or deep gluteal pain syndrome, where the sciatic nerve is compressed by soft tissue rather than spinal structures. Piriformis syndrome accounts for an estimated 5% to 8% of lower back pain cases, and evidence suggests that conservative treatments including exercise and physiotherapy are effective in over 40% of piriformis syndrome patients. Acupuncture is another complementary approach offered at CK Physio, with emerging evidence suggesting it may improve treatment effectiveness for sciatica (risk ratio 1.23), though further high-quality research is needed.
Frequently Asked Questions About Physiotherapy for Sciatica
Can physiotherapy cure sciatica?
Physiotherapy does not "cure" sciatica in the medical sense, but it is highly effective at resolving symptoms and addressing the underlying cause. Around 60% of patients recover within six weeks with structured physiotherapy, and the majority of remaining cases improve within three to six months. CK Physio's personalised treatment programmes target both pain relief and the mechanical factors contributing to nerve compression.
How many physiotherapy sessions will I need for sciatica?
Most sciatica patients benefit from six to twelve physiotherapy sessions over an eight-to-twelve-week period, depending on severity and underlying cause. CK Physio's Chartered Physiotherapists reassess progress at regular intervals and adjust your treatment plan accordingly — some patients respond rapidly and need fewer sessions, while complex cases may require extended care.
Is it safe to exercise with sciatica?
Yes — in fact, gentle, appropriate exercise is one of the most important parts of sciatica treatment. The key is performing the right exercises for your specific condition, as movements that help disc-related sciatica may worsen stenosis-related sciatica. Your CK Physio physiotherapist will prescribe exercises matched to your diagnosis and teach you to perform them safely at home.
Should I see a physiotherapist or go straight to my GP for sciatica?
You can see a physiotherapist directly without a GP referral — CK Physio offers first-contact assessment for sciatica. However, if you have any red flag symptoms (loss of bladder or bowel control, saddle area numbness, sudden bilateral weakness), go to A&E immediately. For non-emergency sciatica, a physiotherapy assessment can begin treatment sooner than the typical GP-to-NHS-physio referral pathway.
Does sciatica come back after treatment?
Sciatica can recur, particularly if the underlying risk factors (weak core muscles, poor posture, sedentary lifestyle) are not addressed. CK Physio's treatment programmes include long-term prevention strategies — strengthening exercises, ergonomic guidance, and self-management techniques — designed to reduce your risk of recurrence significantly.
Can I get physiotherapy for sciatica at home in West London?
Yes. CK Physio provides specialist home visit physiotherapy across Hanwell, Ealing, and surrounding West London areas. Home visits are particularly valuable for acute sciatica when travelling is painful, and allow your physiotherapist to assess and modify your home environment as part of your treatment plan. Call us on 020 8566 4113 or book online.
Ready to Get Relief from Sciatica?
Whether you need clinic-based treatment or a home visit, CK Physio's Chartered Physiotherapists have been helping West London recover from sciatica since 2003. Let us create a personalised plan to get you moving again.
CK Physio Team
Chartered Physiotherapists, CK Physiotherapy
The CK Physiotherapy team comprises expert Chartered Physiotherapists serving Hanwell, Ealing, and West London since 2003. HCPC-registered and CSP members, our team specialises in holistic, personalised care — from in-clinic treatments to home visits.
Sources: NICE NG59 Low Back Pain and Sciatica Guideline, Chartered Society of Physiotherapy, Health and Care Professions Council, Dimitrijević et al. 2025 (PMC), Ridsdale et al. 2025 (PMC), Mann et al. 2023 (StatPearls)

The CK Physiotherapy team comprises expert Chartered Physiotherapists serving Hanwell, Ealing, and West London since 2003. HCPC-registered and CSP members, our team specialises in holistic, personalised care — from in-clinic treatments to home visits.
Latest Blogs







.svg)
.svg)