

18. May 2023
back pain when sneezing: causes, red flags & how physiotherapy helps
If your back hurts when you sneeze, the sneeze itself isn't usually the problem — it's exposing something underneath. A forceful sneeze spikes the pressure inside your abdomen and discs by 35–40% in less than 150 milliseconds, so if you already have a muscle strain, disc bulge, or irritated nerve, that jolt triggers sharp pain in your back, chest, or ribs. The good news: once a chartered physiotherapist identifies the underlying cause, most people recover in 4–8 weeks with the right hands-on treatment and exercises.
Key Takeaway
Pain when sneezing is a diagnostic clue, not a random event. Sneezing raises intra-abdominal pressure to 120–180 cmH₂O and increases lumbar disc pressure by 35–40% — enough to aggravate a strain, disc bulge, sciatica, or intercostal injury that was already there. Physiotherapy (manual therapy + targeted exercise) resolves the underlying condition rather than just masking the pain. At CK Physio in West London, we've treated thousands of patients with sneeze-triggered pain across Hanwell and Ealing — including home visits for patients who find travel difficult.
100 mph
Sneeze Velocity
Peak gas-cloud speed during a forceful sneeze (Bourouiba, MIT)
35–40%
Disc Pressure Spike
Lumbar intradiscal pressure increase during a sneeze
18–25%
UK Hay Fever
Adults with allergic rhinitis (Allergy UK, 2023)
4–8 wks
Typical Recovery
With physiotherapy for acute lumbar strain (Cochrane)
As chartered physiotherapists registered with the Health and Care Professions Council (HCPC) and the Chartered Society of Physiotherapy (CSP), we treat sneeze-related pain almost every week in our Hanwell clinic. It comes up across every age group — from postnatal mothers who've just returned to running, to hay fever sufferers mid-pollen season, to elderly patients with reduced bone density. The mechanism is the same; the underlying condition varies.
This guide explains the physiology behind the pain, walks through the conditions most commonly aggravated by a sneeze, sets out the red-flag warning signs that need urgent assessment, and shows you exactly how physiotherapy can resolve it — often without medication or injections.
Why does my back hurt when I sneeze?
Your back hurts when you sneeze because sneezing creates a sudden, forceful spike in abdominal and spinal pressure that temporarily aggravates an underlying condition — usually a muscle strain, disc bulge, irritated nerve, or intercostal strain. The sneeze isn't causing new damage; it's loading an already sensitised structure. Once your physiotherapist identifies and treats that underlying cause, the pain with sneezing resolves too.
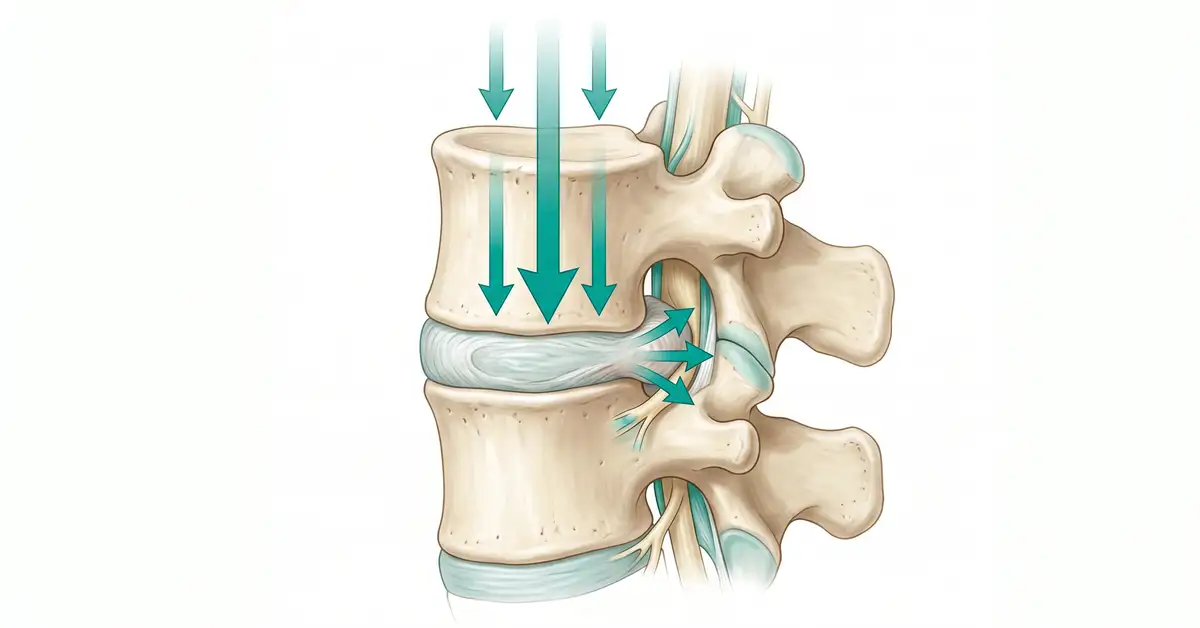
Sneezing transmits sudden downward and outward force through the lumbar discs — enough to aggravate an existing bulge or tear.
A sneeze is one of the most biomechanically violent things your body does — and it's involuntary, so you get no time to brace. In roughly 150 milliseconds your nervous system triggers a three-phase reflex:
- Inspiration (≈50 ms): Your diaphragm drops, lungs fill rapidly, and abdominal pressure begins to rise.
- Compression (≈50 ms): Your glottis snaps shut while your expiratory muscles contract isometrically. Pressure inside your chest and abdomen builds explosively.
- Expulsion (≈50–100 ms): The glottis releases, and air exits at speeds of 100 mph or more (Bourouiba et al., MIT).
During that compression phase, intra-abdominal pressure rockets to 120–180 cmH₂O — comparable to a heavy Valsalva strain (Hodges et al., Journal of Biomechanics, 2001). That pressure is transmitted through the thoracolumbar fascia and loads the lumbar discs, facet joints, and intercostal muscles in one hit. Wilke and colleagues (2001) showed lumbar intradiscal pressure jumps by 35–40% during Valsalva-equivalent events, enough to shift an existing disc bulge further against a nerve root.
That's why sneezing exposes injuries rather than causing them. A healthy spine absorbs the load comfortably. A compromised one doesn't.
Which conditions cause pain when you sneeze?
In most patients, pain on sneezing is caused by one of seven underlying conditions: lumbar muscle strain, disc bulge or herniation, sciatica, intercostal muscle strain, thoracic facet irritation, costochondritis, or (in older adults with reduced bone density) a rib or vertebral stress fracture. A physiotherapist identifies the specific cause through a movement-based assessment — the treatment depends entirely on which one it is.
Here's how each presents — and why the sneeze makes it hurt.
1. Lumbar muscle strain
The most common cause we see in clinic. Strained paraspinal or quadratus lumborum muscles feel manageable at rest, but a sneeze forces a sudden isometric contraction that aggravates the damaged fibres. Patients describe a "catch" in the lower back, usually to one side of the spine. Acute lumbar strain affects around 40% of UK adults each year (British Pain Society, 2020), and 60–70% of uncomplicated cases resolve in 2–4 weeks with early mobilisation and targeted physiotherapy.
2. Lumbar disc bulge or herniation
If you have a disc bulge at L4/L5 or L5/S1, sneezing is the classic trigger. The 35–40% pressure spike temporarily pushes disc material further against the posterior annulus or nerve root, producing sharp back pain that may radiate into the buttock or leg (this radiation distinguishes it from simple muscle strain). A positive Valsalva sign — where the pain reliably reappears when you cough, sneeze, or strain — is one of the stronger clinical indicators of disc involvement. The good news: around 70–80% of symptomatic disc herniations resolve with conservative physiotherapy over 12 weeks (Cochrane Systematic Review, 2021) — most people never need surgery.
3. Sciatica / lumbar radiculopathy
Sciatica describes pain that follows the path of the sciatic nerve, radiating from the lower back through the buttock and down one leg — sometimes as far as the foot. When the nerve root is already compressed (usually by a disc bulge), sneezing spikes epidural venous pressure and mechanically stretches the dural sleeve around the nerve, producing shooting pain, tingling, or numbness. If your leg symptoms consistently worsen when you sneeze, cough, or bear down, that's a strong indicator that the nerve root is involved. Our full physiotherapy for sciatica guide walks through the diagnostic process and evidence-based treatment pathway.
4. Intercostal muscle strain
The intercostal muscles between your ribs contract forcefully during the expulsive phase of a sneeze. If they're already strained — often from exercise, heavy lifting, or prolonged coughing during a chest infection — sneezing produces sharp, localised rib-cage pain that's frequently mistaken for a cardiac issue. The giveaway: intercostal pain is reproducible with palpation between specific ribs and worsens with deep breathing or twisting. Pain that doesn't respond to pressing on the rib cage warrants a same-day GP assessment to rule out cardiac or pleural causes.
5. Thoracic facet irritation
Less common but frequently missed. The mid-back facet joints (T4–T8) can be acutely irritated when a sneeze combines chest expansion with even slight rotation — especially in patients with desk-based postures and an underlying muscle imbalance or forward-head posture. Pain sits next to the spine between the shoulder blades and may refer around the chest wall. Manual mobilisation and postural retraining typically resolve it in 4–6 weeks.
6. Costochondritis
Inflammation at the junction where your rib cartilage meets the sternum. Costochondritis accounts for 10–20% of musculoskeletal chest-wall pain presentations and often follows a viral chest infection or period of intense coughing. Sneezing triggers it because the forceful rib movement strains the inflamed cartilage. It's reassuringly benign — NSAIDs, activity modification, and hands-on treatment usually settle it within 4–12 weeks.
7. Rib or vertebral stress fracture (vulnerable populations only)
In adults with reduced bone density — particularly post-menopausal women, people on long-term corticosteroids, or those with a cancer history — a forceful sneeze can occasionally cause a small rib stress fracture or osteoporotic vertebral compression fracture. Approximately 1 in 3 women over 70 has underlying osteoporosis. Pain is sharp, localised, and often more severe than a simple strain. This is an important red flag scenario — we cover it in detail below.
How each condition presents: a physiotherapist's quick guide
Use this table as a starting point, not a diagnosis. A chartered physiotherapist confirms the cause through movement tests, neurological screening, and — where clinically indicated — imaging referral.
| Condition | Where it hurts | Classic sign | Typical recovery |
|---|---|---|---|
| Lumbar muscle strain | One-sided lower back, paraspinal | "Catch" with rotation or bending; no leg pain | 2–4 weeks |
| Disc bulge / herniation | Central or one-sided lower back ± leg | Positive Valsalva sign; worse with flexion | 6–12 weeks |
| Sciatica / radiculopathy | Back + shooting pain down one leg | Pain follows dermatomal pattern; positive SLR | 4–12 weeks |
| Intercostal strain | Between specific ribs, unilateral | Reproducible on palpation; worse deep breath | 3–6 weeks |
| Thoracic facet irritation | Mid-back, next to spine, T4–T8 | Worse with rotation / extension | 4–6 weeks |
| Costochondritis | Front of chest, costal margin | Tender on costochondral junction | 4–12 weeks |
| Rib / vertebral fracture | Sharp, focal, severe | History of osteoporosis / steroids | 6–12 weeks (after imaging) |
Hay fever, frequent sneezing and cumulative strain
If you sneeze 30 or 40 times a day during hay fever season, your spine is absorbing that load repeatedly — and cumulative micro-strain is the reason many allergy sufferers experience worsening back pain during pollen peaks. Managing the allergy is therefore part of managing the pain.
Allergic rhinitis — hay fever — affects around 18–25% of UK adults (Allergy UK, 2023), with the grass pollen season (May–July) hitting hardest. Someone with moderate symptoms may sneeze 15 times a day; uncontrolled cases routinely exceed 30–50 sneezes daily. For a patient with an underlying lumbar strain or disc sensitivity, this creates a frustrating loop:
- Repeated Valsalva-type pressure spikes fatigue the deep stabilisers (transversus abdominis, multifidus).
- Inflammatory cytokines released during the allergic response lower pain thresholds.
- Muscles become guarded and tense, which makes the next sneeze more painful still.
Breaking the cycle means treating both sides: your GP can prescribe effective non-drowsy antihistamines and intranasal corticosteroids (both reduce sneeze frequency substantially), while your physiotherapist addresses the musculoskeletal sensitivity that allows the repeated sneezing to hurt in the first place. For many West London patients, early action before the pollen count peaks produces the best season overall.
Red flags: when pain after sneezing needs urgent assessment
⚠ Seek same-day GP or A&E review if any of the following develop after a sneeze:
- Loss of bladder or bowel control, numbness around the saddle/groin area, or inability to urinate — these are signs of cauda equina syndrome and require emergency MRI within hours (NICE NG59).
- Progressive weakness in the legs or feet (dropping your foot when walking, inability to stand on tiptoes).
- Severe focal pain in an older adult with osteoporosis, a cancer history, or recent long-term steroid use — may suggest vertebral compression fracture.
- Unexplained fever, night sweats, or weight loss alongside new back pain — rare but important signs of infection or malignancy.
- Severe chest pain with breathlessness after a very forceful sneeze — rib fracture or pneumothorax needs imaging.
- Any sudden, severe, "worst ever" headache triggered by a sneeze or cough.
These presentations are rare — the vast majority of sneeze-triggered pain is mechanical and resolves with physiotherapy — but they need to be excluded early.
How do I stop my back hurting when I sneeze?
The most reliable way to stop your back hurting when you sneeze is to treat the underlying condition — a physiotherapist does this through hands-on manual therapy, graded exercise, and postural retraining. Short-term, you can also reduce the strain each sneeze places on your spine by bracing your core, supporting your back, and avoiding a flexed posture at the moment of expulsion.

Core stabilisation with a chartered physio — bird-dog teaches your body to brace before it needs to.
Brace before the sneeze (when you can)
When you feel a sneeze coming, actively tighten your lower abdominals as if bracing for a punch, keep your spine neutral, and — if possible — place one hand on a stable surface. Avoid bending forward. This sounds minor, but a braced core reduces spinal shear significantly.
Sit or stand tall — never sneeze flexed
A sneeze taken in a flexed, slouched, or rotated position loads the disc at up to 1.5–2.0 MPa (Nachemson, 1981) — nearly double a neutral standing sneeze. Patients who sneeze repeatedly in bed or slumped at a desk often experience worse symptoms because of this.
Treat the allergy
If hay fever is driving frequent sneezing, speak with your GP about modern non-drowsy antihistamines and nasal corticosteroid sprays — both are highly effective at reducing sneeze frequency and let the musculoskeletal system recover between episodes.
Build genuine core stability
Strengthening your deep stabilisers — transversus abdominis, multifidus, diaphragm, pelvic floor — teaches your body to pre-contract before any sudden load, including sneezes. Hodges and colleagues demonstrated that patients with low back pain show a 100–110 ms delay in transversus abdominis activation compared with healthy controls; 8–12 weeks of targeted motor control training restores that timing. Cochrane reviews show core-based programmes cut 12-month recurrence rates by roughly 50%.
How physiotherapy treats sneeze-related back pain
At CK Physio, we treat sneeze-triggered pain through a structured four-phase pathway: assessment and diagnosis, hands-on pain relief, graded exercise, and return-to-function. The majority of patients are substantially better within six visits.
Manual therapy to the thoracic spine and intercostal muscles — often produces noticeable relief within 1–2 sessions.
The evidence supporting this approach is strong. The 2021 JOSPT Clinical Practice Guideline for low back pain places manual therapy combined with exercise as first-line treatment, with pain reductions of 20–25 mm on a 100 mm VAS and a number-needed-to-treat of 5–7 for 50% pain relief (Delitto et al., JOSPT, 2021). Cochrane systematic reviews consistently show this combined approach outperforms passive treatment, medication alone, or exercise alone.
PHASE 1 · WEEK 1
Assessment & pain relief
Detailed history, movement tests, neurological screen (reflexes, myotomes, dermatomes), and postural analysis. Initial hands-on techniques — soft tissue release, gentle joint mobilisation — to reduce acute guarding.
PHASE 2 · WEEKS 2–3
Manual therapy & early exercise
Progressive manual therapy (mobilisation, manipulation where appropriate), directional preference exercises (McKenzie-style where indicated), and initial core activation work.
PHASE 3 · WEEKS 4–6
Graded loading
Integrated core stability (bird-dog, dead bug, plank progressions), postural retraining, and gradual return to normal activity. Ergonomic advice for desk, driving, and sleep positions.
PHASE 4 · WEEKS 6–12
Prevention & return to sport
Sport- or task-specific progression, plyometric or resistance loading where appropriate, and a home maintenance programme to keep recurrence rates low through the next allergy season.
The techniques we use most often
Depending on the diagnosis, your treatment may include manual therapy and soft tissue release, joint mobilisation or manipulation, electrotherapy or TENS for acute pain control, shockwave therapy for chronic tendinopathy-related intercostal pain, and medical acupuncture. We also draw on therapeutic ultrasound and holistic, whole-body assessment — because treating just the painful segment without fixing the pattern rarely holds.
Home visits for patients who can't travel

Our home visit physio service — coaching a patient on correct sneeze bracing technique in her own front room.
When back pain from sneezing is severe enough that travelling is painful, or when you're caring for an older parent with reduced mobility, a clinic appointment often isn't realistic. CK Physio offers chartered physiotherapy home visits across Hanwell, Ealing, Acton, and wider West London. We bring the treatment couch, electrotherapy equipment, and assessment tools to you, and we use the home setting constructively — coaching you on the exact chair, mattress, and workstation ergonomics that may be contributing to the problem.
Home visits are particularly valuable for elderly patients (where falls risk and osteoporosis complicate the picture), postnatal mothers, patients recovering from surgery, and anyone in acute pain. Our full home visit physiotherapy guide explains how it works, who it's suitable for, and pricing.
Frequently asked questions
Why does my back hurt when I sneeze?
Your back hurts when you sneeze because the sudden spike in intra-abdominal and intradiscal pressure — a 35–40% increase in under 150 milliseconds — aggravates an existing condition underneath. In most cases that condition is a lumbar muscle strain, disc bulge, or irritated nerve. The sneeze isn't causing new damage; it's exposing something that needs treatment.
Can sneezing cause a slipped disc?
Sneezing alone is very unlikely to cause a disc herniation in a healthy spine. However, if you already have a weakened or degenerate disc, the pressure spike during a forceful sneeze can push existing bulge material further against the nerve root, producing new radiating pain or worsening sciatica. Around 70–80% of disc herniations resolve with conservative physiotherapy without the need for surgery.
Is it normal for sneezing to cause chest pain?
Chest pain when sneezing is most commonly caused by an intercostal muscle strain or costochondritis (inflamed rib cartilage), both of which are benign and respond well to physiotherapy. However, if chest pain is severe, radiates to your arm or jaw, is accompanied by breathlessness, or doesn't reproduce with direct palpation of the ribs, seek same-day medical advice to rule out cardiac or pulmonary causes.
Can hay fever make back pain worse?
Yes. Allergic rhinitis — which affects 18–25% of UK adults — causes repeated bouts of sneezing, and cumulative Valsalva-type pressure spikes fatigue the deep spinal stabilisers. Inflammatory cytokines released during the allergic response also lower pain thresholds. Many of our patients notice a clear flare during the May–July grass pollen peak. Treating the allergy (antihistamines, nasal corticosteroids) alongside the musculoskeletal cause typically resolves both.
How do I stop my back from hurting when I sneeze?
Short-term: brace your core before the sneeze, sneeze standing or sitting tall rather than bent over, and manage any allergies driving the sneeze frequency. Long-term: see a chartered physiotherapist to diagnose and treat the underlying condition (muscle strain, disc bulge, or nerve irritation) and build core stability to absorb future loading. Most patients are substantially better within six physiotherapy sessions.
When should I see a physiotherapist about pain when I sneeze?
Book an assessment if the pain happens every time you sneeze, is getting worse rather than better, radiates into a leg or arm, or is stopping you sleeping or working. You don't need a GP referral to see a private chartered physiotherapist — and at CK Physio we offer same-week appointments, evenings, Saturdays, and home visits across West London. If you have any red flags (loss of bladder/bowel control, progressive leg weakness, fever, unexplained weight loss, severe focal pain with osteoporosis history), seek same-day GP or A&E review first.
How many physio sessions will I need?
For acute lumbar muscle strain triggered by a sneeze, most patients need 3–6 sessions over 4–6 weeks. For a disc bulge or sciatica, expect 6–10 sessions over 8–12 weeks. Costochondritis and intercostal strain typically resolve in 4–6 sessions. Your physiotherapist will give you a clear estimate after the initial assessment, and we review progress every 3–4 visits to make sure the plan is still the right one.
Book an assessment at CK Physio
If your back, chest, or ribs hurt when you sneeze, it's worth finding out why — early, evidence-based physiotherapy resolves most causes in weeks rather than months. Our chartered physiotherapists in Hanwell and Ealing have been treating sneeze-triggered pain for over 22 years, and we're registered with BUPA, AXA Health, Vitality, and all major private insurers.
Back pain when you sneeze? Let's fix the underlying cause.
Chartered physiotherapists in Hanwell & Ealing. Clinic or home visits across West London. Same-week appointments, BUPA / AXA / Vitality registered.
or call 020 8566 4113 · contact us
Clinically reviewed by the CK Physio team
Chartered physiotherapists, HCPC-registered, CSP members. Serving West London since 2003 — thousands of patients across Hanwell, Ealing, Acton, Greenford, Brentford & Ruislip.
Sources & further reading: Bourouiba L et al. Violent expiratory events, Journal of Fluid Mechanics (2014); Hodges PW et al. In vivo measurement of intra-abdominal pressure on the human spine, Journal of Biomechanics (2001); Wilke HJ et al. New in vivo measurements of pressures in the intervertebral disc, Spine (2001); Delitto A et al. Low Back Pain Clinical Practice Guidelines, JOSPT (2021); NICE NG59 Lower back pain and sciatica (2016); Allergy UK rhinitis prevalence report (2023); Chartered Society of Physiotherapy; Health and Care Professions Council; Cochrane Collaboration systematic reviews on manual therapy and motor control exercise (2015–2021). Clinically reviewed by the CK Physiotherapy team. trapped nerves in the neck and shoulders complete postnatal physiotherapy guide whiplash and neck injury recovery
Latest Blogs








.svg)
.svg)