

12. June 2017
sciatica pain relief: how physiotherapy helps | ck physio
Sciatica affects an estimated 13.5% of the UK population at some point in their lives. It occurs when the sciatic nerve — the longest nerve in your body, running from your lower back down through each leg — becomes compressed or irritated, causing radiating pain, numbness or tingling. The good news: physiotherapy is an effective first-line treatment, with 80–90% of patients achieving full recovery within 6–12 weeks through targeted exercises and hands-on therapy.
Key Takeaway
NICE guidelines (NG59) recommend physiotherapy — specifically exercise therapy combined with manual therapy — as the primary treatment for sciatica. Surgery is reserved for severe or persistent cases. Most patients see meaningful improvement within 2–4 weeks, and long-term outcomes from physiotherapy are comparable to surgery for the majority of cases.
What Is Sciatica and What Causes It?
Sciatica describes pain that radiates along the path of the sciatic nerve, which branches from your lower back through your hips and buttocks and down each leg. The pain typically affects only one side and can range from a dull ache to a sharp, burning sensation that some patients describe as feeling like an electric shock.
The most common causes of sciatic nerve compression include a herniated (slipped) disc pressing on the nerve root, spinal stenosis (narrowing of the spinal canal), piriformis syndrome where the piriformis muscle in your buttock tightens and irritates the nerve, and degenerative disc disease. Less commonly, sciatica can result from pregnancy, spinal tumours or injury.
Common symptoms include pain radiating from your lower back through your buttock and down the back of your leg, numbness or tingling in your leg or foot, muscle weakness that makes it difficult to move your leg or foot, and pain that worsens when sitting, coughing or sneezing. If you experience sudden loss of bladder or bowel control, progressive weakness in both legs, or numbness in the groin area, seek immediate medical attention — these may indicate cauda equina syndrome, a medical emergency.
13.5%
of the UK population affected
80–90%
recover with conservative treatment
6–12 wks
typical recovery with physiotherapy
How Does Physiotherapy Treat Sciatica?
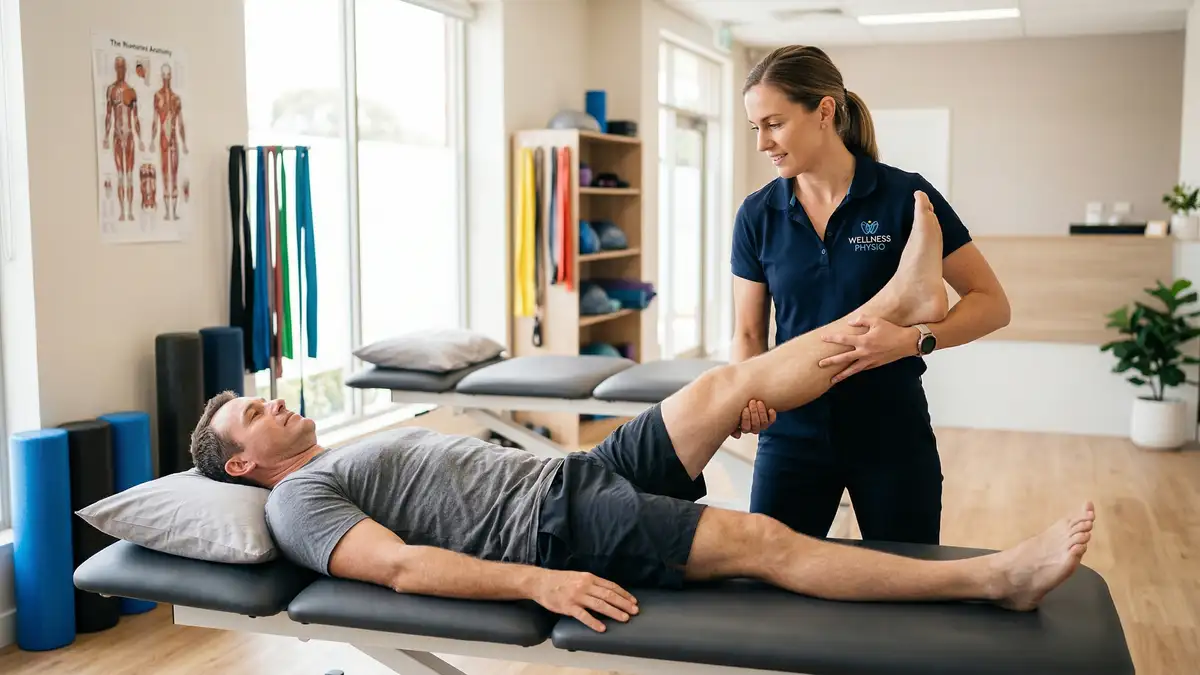
Physiotherapy takes a multifaceted approach to sciatica, addressing both the pain and the underlying cause of nerve compression. NICE guidelines recommend that treatment should be tailored to each patient using risk stratification tools like the STarT Back questionnaire, which helps your physiotherapist determine the right intensity of treatment for your specific situation.
Reducing Nerve Compression with Manual Therapy
Your physiotherapist will use hands-on techniques to relieve pressure on the sciatic nerve. These include spinal mobilisation — gentle movements that improve joint mobility and create more space for the nerve — as well as soft tissue mobilisation to release muscle tension in the lower back, buttocks and legs. For piriformis syndrome, targeted deep tissue work on the piriformis muscle can provide significant relief. NICE recommends that manual therapy should always be combined with exercise rather than used as a standalone treatment.
Strengthening Supporting Muscles
Weak core, back and hip muscles put additional strain on your spine and sciatic nerve. Your physiotherapist will prescribe targeted strengthening exercises to stabilise your spine and pelvis, build strength in the muscles that support your lower back, and improve hip and leg stability to correct imbalances that contribute to nerve compression. Core stabilisation exercises have the strongest evidence base for both treating and preventing recurrence of sciatica.
Improving Flexibility Through Stretching and Nerve Gliding
Tight muscles — particularly the hamstrings, hip flexors and piriformis — can worsen sciatica by placing additional tension on the sciatic nerve. Your treatment plan will include targeted stretches for these muscle groups, along with neurodynamic (nerve gliding) exercises that gently mobilise the sciatic nerve along its path, reducing irritation and improving nerve function. Nerve gliding should be performed gently — aggressive stretching can aggravate an already irritated nerve.
Complementary Modalities
Depending on your symptoms, your physiotherapist may incorporate additional treatments such as electrotherapy or TENS for pain management, shockwave therapy where muscle tension contributes to nerve compression, or acupuncture for additional pain relief. These work alongside the core programme of exercise and manual therapy to accelerate your recovery.
Sciatic pain limiting your daily life?
Our chartered physiotherapists specialise in diagnosing the root cause of sciatica and creating personalised treatment plans.
Book Your AssessmentPhysiotherapy Exercises for Sciatica
While your physiotherapist will tailor an exercise programme to your specific condition, the following exercises are commonly prescribed for sciatica. Always perform them within your pain tolerance — a gentle stretch is fine, but sharp or shooting pain means you should stop and consult your physiotherapist.
1. Knee to Chest Stretch
Lie on your back with both knees bent and feet flat on the floor. Gently pull one knee towards your chest using both hands, keeping your lower back pressed to the floor. Hold for 30 seconds, feeling a stretch through your lower back and hip. Slowly lower and repeat with the other leg. Perform 3 repetitions on each side. This stretch relieves tension in the lower back and hip, reducing pressure on the sciatic nerve.
2. Sciatic Nerve Glide
Sit upright on a chair with both feet flat on the floor. Slowly straighten one leg while pointing your toes toward the ceiling and looking upward. Then bend the knee back down while tucking your chin to your chest. Move smoothly between these two positions for 10 repetitions on each side. This gentle nerve mobilisation helps the sciatic nerve glide more freely, reducing irritation without aggressive stretching.
3. Glute Bridge
Lie on your back with knees bent and feet flat on the floor, hip-width apart. Tighten your core and squeeze your glutes, then raise your hips until your body forms a straight line from shoulders to knees. Hold for 3–5 seconds at the top, then slowly lower back down. Perform 2 sets of 10 repetitions. This exercise strengthens the glutes and core muscles essential for spinal stability. As you progress, try single-leg bridges for an added challenge.
4. Piriformis Stretch (Figure-4)
Lie on your back with both knees bent. Cross your affected leg over the other so your ankle rests just above the opposite knee, forming a figure-4 shape. Gently pull the bottom leg toward your chest until you feel a deep stretch in the buttock of the crossed leg. Hold for 30 seconds and repeat 3 times. This stretch targets the piriformis muscle, which can compress the sciatic nerve when tight — a common contributor to sciatica symptoms.
5. Bird Dog
Start on your hands and knees with your back flat. Simultaneously extend your right arm forward and your left leg backward, keeping your hips level and core engaged. Hold for 3–5 seconds, then return to the starting position. Repeat with the opposite arm and leg. Perform 2 sets of 10 repetitions per side. This exercise builds core coordination and spinal stability, which are fundamental to preventing sciatica recurrence.
Physiotherapy vs Surgery: What Does the Evidence Say?
For the vast majority of sciatica patients, conservative treatment with physiotherapy is the appropriate first step. Research consistently shows that 80–90% of cases resolve without surgery, and long-term outcomes at 1–2 years are comparable regardless of whether patients chose the surgical or conservative route.
Surgery does offer faster initial pain relief — patients typically experience significant improvement within days to weeks rather than weeks to months. However, physiotherapy patients show superior quality of life outcomes at the 1–2 year mark for leg pain, with a lower risk profile and lower cost.
NICE guidelines recommend considering surgical referral when symptoms are severe or worsening after 6–12 weeks of appropriate physiotherapy, when there is progressive neurological deficit such as foot drop or increasing weakness, or when pain significantly disables work, sleep or daily activities despite conservative treatment. Your physiotherapist can monitor your progress and recommend specialist referral if needed.
How Long Does Sciatica Take to Heal?

Recovery timelines vary depending on the underlying cause and severity, but structured physiotherapy significantly accelerates healing compared with rest alone. Around 75% of patients experience meaningful improvement within 4 weeks, and most achieve full recovery within 6–12 weeks with consistent treatment. Acute episodes often respond within 1–2 weeks to a combination of gentle movement, manual therapy and targeted exercises.
Chronic sciatica (symptoms lasting longer than 12 weeks) typically requires a more comprehensive approach, potentially combining exercise with manual therapy and psychological support as recommended by NICE. The key message: staying active and following your prescribed exercise programme will give you the best chance of a quick and lasting recovery. Prolonged bed rest is not recommended and may actually slow healing.
Can Sciatica Be Treated at Home?
Severe sciatica can make travelling to a clinic extremely difficult — sitting in a car often worsens the pain. This is where home visit physiotherapy can be particularly valuable. A physiotherapist can come to your home to perform a thorough assessment, develop a personalised exercise programme, evaluate your furniture and sleeping setup, and monitor your progress without requiring you to travel while in pain.
CK Physiotherapy offers home visits across Hanwell, Ealing and wider West London. For many sciatica patients, the initial assessment and first few treatment sessions at home — followed by clinic visits as mobility improves — provides the optimal recovery pathway.
Frequently Asked Questions
| Should I rest completely with sciatica? | No. Brief rest during acute flare-ups is fine, but prolonged bed rest is not recommended. Gentle movement and prescribed exercises maintain flexibility, reduce muscle tension and promote healing. Your physiotherapist will help you find the right balance between rest and activity. |
| Can sciatica come back after treatment? | Yes, sciatica can recur, particularly if the underlying cause is not addressed. Your physiotherapist will teach you a maintenance exercise programme, proper posture techniques, and lifting methods to significantly reduce the risk of recurrence. |
| Can I work with sciatica? | Most people can continue working with appropriate modifications. Your physiotherapist can recommend ergonomic adjustments, regular movement breaks, and desk stretches. If your job involves heavy lifting or prolonged sitting, you may need temporary modifications during recovery. |
| Is walking good for sciatica? | Gentle walking is generally beneficial and helps maintain mobility. Start with short, comfortable distances and gradually increase as symptoms improve. If walking worsens your pain, discuss alternative movement options with your physiotherapist. |
| How do I sleep with sciatica? | Sleeping on your side with a pillow between your knees can reduce pressure on the sciatic nerve. If you prefer sleeping on your back, placing a pillow under your knees helps maintain the natural curve of your spine. Your physiotherapist can recommend the optimal position for your specific condition. |
| When should I seek urgent medical attention? | Seek immediate medical care if you experience loss of bladder or bowel control, progressive weakness in one or both legs, numbness in the groin or saddle area, or severe pain that worsens rapidly despite treatment. These may indicate cauda equina syndrome, which requires emergency assessment. |
Get Expert Help for Your Sciatica
Our HCPC-registered physiotherapists in Hanwell and Ealing have over 22 years' experience treating sciatic pain. We offer flexible appointments including early morning, late evening and Saturday slots — plus home visits across West London for patients who cannot travel comfortably.
Book Your Assessment TodayBUPA and AXA PPP registered · No GP referral needed
Sources: NICE Guideline NG59 — Low Back Pain and Sciatica in Over 16s; NHS Sciatica guidance; Chartered Society of Physiotherapy; systematic reviews on physiotherapy vs surgical outcomes for sciatica; UK prevalence data.
Conditions we treat · Sciatica and electrotherapy · Pinched nerve treatment · Lower back exercises · Mobility assessment
Latest Blogs








.svg)
.svg)